Uncategorized – Read All Articles
So, I’ve Had a Long Writing Hiatus
Hi!
So, today is February 21st, today is the day when medical students submit their match list. In case it’s not abundantly clear, I’m applying to neurology. Though, for half of MS3 I seriously considered Ob/Gyn but had a change of heart after having a neurology rotation. I just put mine in a few days ago, and I’ve already cracked open a bottle of alcohol to celebrate. Now comes the waiting game, on March 16th at 12 pm EST all successfully matching medical students will open their a letter that’ll tell us where we’ll do our residency.
I believe the last post I had I just finished my third-year medicine rotation. Since that time, a lot of things have happened. I took and passed STEP 2 CS and CK, applied to residency, interviewed at 12 programs, tackled a rather random 4th-year schedule (thus far I’ve done ambulatory medicine, headache/pain clinic, stroke inpatient sub-internship, TA’d anatomy, medicine sub-internship, project I worked on a few years ago got published, now I’m working on a poster presentation at the moment, and all while trying to be a decent husband to my wife. As such, posting on my blog has somewhat taken a backseat.
The goal of this post is just to touch bases with those who’ve been reading for awhile and maybe address a few things that have come up during conversations with MS2’s who worry about the year to come of MS3. Should you want a specific topic, just let me know and I’ll either direct message you or turn it into a blog post if it seems generalizable. In fact, most tips are rather general so I have a twitter thread already going with (useful?) tips: https://twitter.com/doctorORbust/status/869652425875083264
Should you have any questions just let me know. Hopefully, now I’ll have a little more time to post more regularly. One of the biggest mysterious now is will my website/screen name change, after all, I’m going from “doctor or bust” to “definitely a doctor.” Thanks for being there during my transformation, friends.
Patient Reflection: Internal Medicine
“You’re not cutting it off, I don’t care if I die…”
Ms. Marrow lay tired, her facial expression sullied with fatigue, left arm gnarled tubes bringing her tainted scarlet tinged blood into the machine keeping her alive. Ms. Marrow, another victim of the end stage complications associated with poorly controlled diabetes: end-stage renal disease with dialysis dependence, stocking distribution neuropathy (loss of proprioception, touch, and intermittent sharp searing pain), and previous strokes. Angry at her disease, frustrated at her seemingly inexplicable decent in health, and now uncertain of her fate. Recalcitrant towards healthcare system, askance towards medical explanations, her own illness and experience left her skeptical of our “good intentions.” As a patient, she was said to be difficult and infamously inapproachable. Deep down, she was scared and understandably so, for in her body lay a harbinger of doom. And for several days, I would try to work to earn her trust so I could convince her to let us sever off her foot.
Her foot was dying, skin peeling, from sole to heel her violaceous flesh split in two to drain her festering infection from multiple organisms. Though, obscuring the seriousness of Ms. Marrow’s medical risk was her unremarkable temperature, heart rate, and blood pressure. From her own gestalt, she had drawn the conclusion that she’d be fine. But, it was all a subterfuge. Ms. Marrow’s had “diabetic foot”, an etiologic triad of ischemia, neuropathy, and infection. Yet alas, the most difficult person to save is the one who thinks everything is fine.
Our fear as a medical team, though appeared fine on the outside, she’d eventually reach a tipping point and slip into a point of no return – this year, I’ve seen people come back from the brink, but it’s always been at an incalculable price.
She required an amputation, without the procedure she would likely not only lose the foot but also her life but a life-saving surgery that she adamantly refused. Against medical advice, Ms. Marrows decided that she would only be amenable to medical treatment, there was to be no amputation. No doubt, her stable vitals signs only served to obstinate the problem of ridding her of her poisonous limb. So, we gave her our best drugs and we gave her broad antibiotic coverage (including MRSA), and then we waited. It was a bad plan, a route fraught we pitfalls, but we the patient our captain we temporarily sailed on into the abyss. Like a roll of a loaded cosmic dice, her life would play out in three scenarios 1) by a miracle the foot would heal enough to use, 2) the foot would undergo unlikely innocuous necrosis 3) her infection from her decaying foot would spread to her blood and kill her. The longer we tried antibiotics and bided our time, the likely the bacteria could spread into her bone, and into her blood. The more it the infection creeps, the more flesh should be sacrificed, but at some point, there’s a limit of how much you take to fix the problem of inevitable death.
I spent a few days getting to know Ms. Marrow and she weren’t always in this situation. In fact, this whole situation started as nothing more than a trivial accident. Two weeks prior her arrival to the hospital, she had been in her normal state of health. She was at home, enjoying her independence at the age of 70, where she lives alone. When mentioning her children, she beams with proudness as she recounts how she raised them to be self-sufficient. She has no plans of dying, indeed she plans on getting married to a high school crush in July, loves going to the casino, laments on her recent loss of her “curves”, and recounts how she gets bored of “country people” when visiting her home town in Virginia. She mourns the days where she used to be able to drive, a couple of years ago she gave up driving because she could no longer feel the pedals. Each time we’d meet, she’d share another part of her life with me, sometimes when prompted I’d share some of my life, and each day I would slowly gain her trust. She hated her diabetes, how it changed her, how it aged her, and how it took away who she was. Diabetes had been a scourge to nearly her whole family. Her grandparents had it, as did her parents, as did her brothers and sisters. Two of her brothers with diabetes left a notable impact on her. One brother on dialysis died abruptly, of what the patient said was conditions related to his dialysis. Another brother, he started with toe amputations, which lead to a trans metatarsal amputation, which subsequently leads to a below the knee amputation, and this finally leads to an above the knee amputation. After seeing her brothers, Ms. Marrow distrusted doctors. Her terse talk and cantankerous tone with the medical staff wasn’t borne of ill will or spite but instead came forth from fear and inadequate health literacy. There was a constellation of reasons why Ms. Marrow’s said to use, “You’re not cutting it off, I don’t care if I die if I die it’s the will of God and only he knows what’s supposed to happen.”
While at home, she stepped on something; at the time she didn’t know what it was. But, before she could sit down and inspect her foot a knock on a door lead to a conversation, the conversation lead to laughs, laughs lead to distractions, and distractions lead Ms. Marrow to forget about her foot. After that day, her foot ached, but foot pain is nothing new and her “new” pain was ignored. Eventually, someone noticed Ms. Marrow’s foot and urged her to go the hospital and eventual removal of a sewing needle that was embedded within her.
The source of her brush with demise lay in a tiny metal rod. One morning, a blood result came back that indicated our worse fears. This tiny rod as it plunged into her flesh brought with it the bacteria to where it ought not to be, into her blood despite our optimal antibiotic treatment. The microscopic invaders were no longer a hypothetical threat to her life, instead, now the infection was a tangible assassin laying in wait to take her life. Our attending physician decided to round up the team for a last ditch intervention to convince Ms. Marrow of her perilous situation. She was indifferent towards others so I volunteered, albeit hesitantly, to lead the conversation to be had with Ms. Marrow. That is, a conversation with a definite goal: talk Ms. Marrow into cutting off her foot, and inform her of the possibility that we may need to take more as we’ve waited so long. We let her eat her lunch, when the scrounged up several chairs for us to sit down in while we talked to her. Though I had a chair, I decided to stand by her bedside. It probably appeared as an act of confidence on my part, but in actuality I just wanted to be close to her because I knew soon I would hurt her. I knew soon I would use all that she had trusted me with, the details of her life and goals, and the relationship that we formed to convince her to try to fight to live. From our perspective it would appear noble, from her perspective we were no less vile than her very disease. I stood next to her both to comfort her and to assuage my own concerns of how my word would dig at her soul.
For what felt like an eternity, we talked, debated, she argued, we listened to each, and when she became silent we became silent. The conservation hit what seemed like an unrecoverable dead in several times, each dead end avenue lead to a refusal to even consider surgery. I suppose, in the last act of betrayal of her friendship, I used the last bit of information I knew about Ms. Marrow. I said to her, “I know you don’t like asking for help, but what we are asking is to let us help you.” She broke eye contact with me, and though emotional, never allowed herself to outwardly weep. She said to us, “This is something I’d need to think about.” We all agreed to that as a viable solution for the time being. Angry with us, angry with me, she told us all to leave and not return that day. Ms. Marrow imagined death would be better than becoming dependent on others, she thought death as a tidy way to be done with things. This fly in defiance against her plans to keep living a full live. I often struggled to reconcile how she could both retire herself to death and make concrete near term plans.
A day later, she decided to get the amputation, I hope one day I can update this ending and tell you that she went to her wedding. And I hope that one day I can tell you that I wasn’t wrong, after all there was some truth in Ms. Marrow’s belief that we don’t know everything.
Thank you for reading. This piece was a writing assignment that I submitted during my rotation.
My Neurology rotation over, and breezing thru Surgery.
Hello reader,
First off, belated happy new year. If you’ve stuck with me through all this time, thank you! I started this blog around the time I started applying to medical school. I’m now a 3rd year and on my clerkship rotations. Later this year, I apply for my first job as a doctor.
At the moment, I’m on my general surgery service. I’m on my away rotation away from Boston, the school provides a house near the hospital. I live with two other students from my school, one is on surgery with me, the other is on another rotation. Prior to this rotation, we were all friends, the three of us have a pretty easy going relationship.
On Neurology
What has also been surprising, at least for myself, is that lately I’ve been considering Neurology as a specialty. In context, I haven’t had medicine yet, and my original top choice was leaning towards Ob/Gyn. The reasons are fairly complicated, and probably merits its own discussion. But, one thing I’ve considered is that I have a background in electrophysiology, did well in medical school neuroscience on theory and clerkship, and I had fun. It seems somewhat appropriate to consider it. Really though, who knows what I’ll end up doing, everything have been somewhat “doable.”
Surgery
As I mentioned, right now, I’m on surgery. I just finished 4-weeks of trauma and vascular, hence all that is left is general surgery. While on trauma and vascular, I worked 6-days a week, for a total of about 78-80 hours a week (there’s a rule of not exceeding an average of 80 hrs/week). On this service, there is a week where I’ll go over 80, but the following week I’ll have some time off compensated.
Prior to surgeries, I arrive at around 4:40 AM, I pre-round on my patients (usually three). I write notes on my patients, this hospital uses a paper/computer hybrid system. Sometime before rounds, I have to find their nurses to get the latest updates. To a resident, I present my three patients during 6 AM rounds and make a plan for that patient. Between 7:20AM and 9AM I start scrubbing into surgeries. a few surgeries a day, mostly “driving” the endoscopes, retracting things, occasionally cauterize a bit or two, tie up things, try not to contaminate things, and brave the emotional OR storm – the latter being the most vital to survival.
If I’m out of surgery before 2 or 4 PM, I go to PM rounds with the residents. This time, because other students are in surgeries, I pick up patients who aren’t mine to present. This time, instead of “short rounds” like the morning, PM rounds are just me saying a sentence about a patient to summarize their admission/course. This also acts as “sign-out”, so the overnight resident gets their updates from you. After this, I typically go home, sometimes I go back to surgery. Eventually, because I live really close to the hospital, I make it home rather early 5:30~PM. Besides that, on this service, I had my first weekend in a month. My roommate and I usually leave together, we sit at the dinner table, study, eat, and again start another day. With that being said, I generally like surgery, and I’ve gained the skills I needed to not get eaten alive:
- Be able to read the schedule (it’s harder than you imagine, my kingdom for a schedule that is easy to read and accurate)
- Navigate the electronic medical records at a new hospital
- Get lost less at a new hospital
- Cut surgical strings the correct length and tie decent knots
- Make presentations as short as possible
- Get really good at asking about pee, poop, passing gas, have few qualms asking people to disrobe, and making doorway assessments
Just a few more weeks of surgery, then I’m onto internal medicine: Renal medicine (2 weeks), Hematology/Oncology (2 weeks), and 4 weeks of general medicine. I really was hoping for 2 weeks of Cardiology, but I didn’t get it – I’ll do it as a 4th year, along with emergency medicine.
Two weeks or so after finishing 3rd year, I take STEP 2 CK. Then, during October as a 4th year, I’ll fly out to Chicago to take another exam (the infamous STEP 2 CS). I’ve spent $1,800 so far on just registering for the exam. Good times, eh?
Well, that’s it for me, back to reading. And thanks for reading!
Good Bye to My Best Follower!

There is slight tracheal deviation to the right, the cardiomediastinal silhouette is completely obscured on the right and the mediastinal width is widened in the left lung field. The diaphragm right hemi-diaphram is obscured on the right, while the left diaphragm, costophrenic sulcus obscured on the right and visible on the left. In the right upper lung field, within the opacity, there’s a central lucency.
Given multi-decade smoking history, significant second hand smoke exposure as a child, primary lung cancer should be strongly considered in the differential diagnosis.
…are things I would say, if I didn’t know the identity of this patient.
This X-ray is from last year, from a person I knew, a person who treated me like a son. I haven’t looked at the X-ray for over a year. When his parents died, and left him some money, some of it went towards my education. I used a portion of that money to pay for medical school applications, the rest went to living expenses racked up while moving to New England for said medical school acceptance.
He grew up essentially poor and never had a chance go to college himself, so he always wished his kids would obtain more than he did. His parents owned a model battleship and cigarette shop, an admittedly strange business combination. In Japan, for a family business, it’s not uncommon to both own a space for business and use said space for quarters. The building, his home, was a two-story building with the family living upstairs and the business downstairs. Customers would bustle about, old men recollecting their pasts in miniatures whiles they chain smoked their new purchase. And really, at those times, the effects of second hand smoke were still unknown (to the public). In that house, his little brother and him grew up, it was only his little brother afforded a college education by his parents budget.
Later, he would go onto have two kids of his own. He would go onto encourage his daughter to go to college, she later went onto to get her masters. His daughter traveled to London, then to California, it was in the latter location that we got together. He was tech savvy, so he would be sure to keep up with his daughter several times a month via Skype.
Over time, we got closer. I started to think of him as another dad. When I was still planning on applying to medical school he supported my decision. Prior to medical school, when I had considered a PhD, he also supported my decision. His daughter told me that she had hated, vehemently, any of her previous boyfriends while in Japan. So, I just naturally assumed he’d have a death wish out for me. He didn’t. Instead, he embraced me as a son. He’d brag about my latest conference, tell his friends how I was working hard to make ends meet/further my goals. He even followed my blog and Twitter, at my blog’s inception I hardly had any visitors, so when I saw an IP address from Japan I knew it was him.
I’ll never forget his approving eyes while I would tell him my life plans.
Several weeks prior to the first X-ray shown above, I found out afterwards, he had been experiencing shortness of breath, and hemoptysis (coughing up blood). He walked into a mobile imaging service and got a chest X-ray, a place he usually went to for his yearly chest X-ray. The person who interpreted the image told him, in so many words, “Go home, it’s just pneumonia, it’ll be okay.” Now, I could write a whole other article on the ethics of the paternalistic nature of this decision, but that’s for another day; I could write another article on the fool heartedness of using an X-ray (with CT) to screen a high risk patient for lung cancer. He ignored the advice to just go home, bringing a copy of his X-rays with hm, he visited the hospital that he worked at as an maintenance electrician. They immediately checked him in, he was soon diagnosed with lung cancer.
They began radiation treatment, at the request of the family and patient to give it a good fight. The doctors, they pushed on with great outward reluctance. After a week of treatment, the impression of his X-ray improved somewhat:

However, a few days into his fight, his daughter called me. She told me that he had been talking about complaining to the mayer of the city about the hospital service. He’d often go on long nonsensical rants, stringing together figments of his past life with confabulations. When I was being told this, I was just a second year medical student, I had just learned of the term “delirium”. And, what little I knew of it, I knew it was a bad sign. Over that weekend, in the ICU, at some point of his course of treatment he likely developed a pulmonary embolism. During the night, he struggled for breath, in a bit of confusion ripped his IV and oxygen out, and died sometime in the early morning.
Then, I went back to school, along with my day, as if nothing happened. A few months later, I took my board exam. It was tough to do without him, I think I had imagined he’d be there to cheer me on like he did for the MCAT. Just like how proud I imagined he’d be at my graduation as a MD. Now, when I see my blog stats, I know the Japan location isn’t him – it was a hard truth to swallow. And it’s taken me over a year to slowly soak it all in – during that time, I lost my will to write, and blog posts inevitably slowed down.However, medical education doesn’t allow much time for personal feelings. Knowing about medicine doesn’t necessarily make people dying easier, if anything it makes it colder, more visceral, and unquestionably unforgiving.
It’s been a year now since he passed away, and it’s always hard to let go of your family and biggest cheer leader. As a medical student, as I learn how to become a doctor, I now always reflect that each patient has a rich back story unknown to me. But, their backstory is known well to all of those of love them.
Radiology Rotation – Over

In a nutshell, the diagram above explains your ‘choices’ in the 3rd year of medical school.
This morning, I finished my 4-week Radiology rotation by sitting for my shelf exam. So far, this has been my fifth rotation of the year – I’ve now finished Ob/Gyn, Pediatrics, Psych, Family Med, and Radiology. Next week, I start Neurology. It’s likely that I’ll start on their stroke service for a couple of weeks. From there, I’m not really sure how it works. I may sound in doubt because, as is the nature of my life, I’ve learned to never trust my schedule until it’s printed out on orientation day. After all, 3rd year medical students don’t actually make their schedules, the strings of fate or somewhat pulled from the background. You have some general say in how the game will precede, would you like to fight Hard Man first or Gemini Man? Either way, the end game is completion of a linear experience, we all know there’s going to be that final boss battle (STEP 2).
Radiology was a very fun rotation, for a variety of reasons. I’ll be upfront, a lot of the enjoyable parts of the rotation was the lifestyle. They not only allowed time to be prepared, but they also directly encouraged making time for your personal life. We had time to be human.
Radiology, though fundamental, is most often an optional elective in medical school. Most medical students do not end up taking Radiology. At our program, we had to choose between Radiology, Emergency Medicine (EM), or research. This isn’t to imply that students who took EM didn’t want to benefit from Radiology, because part of the function of 3rd year is to try rotations before we apply during early 4th year, there just wasn’t time for some with definite plans of EM. I’ve never really given EM much thought, I’ll try it during my 4th year as an elective. And, I didn’t have any research projects on the back burner that would justify a research block. To be honest, I’ve been waiting for this rotation since Ob/Gyn.
You see, 3rd year, it’s arguable if your decision of “order” helps all that much. If you have Psychiatry first, well you’ll soon learn there’s a lot of medicine involved. Should you have Family Medicine first, then you’d wish you’d had Ob/Gyn, Pediatrics, Psychiatry, or Medicine beforehand. Either way, you pick up tools, you learn new things on rotations and use them in the others.
The first time I had to attempt reading an radiology image was on my first rotation, Ob/Gyn. It was a pelvic ultrasound, and even though I knew the pelvic anatomy down cold, to be honest I had no idea what I was looking at on the screen. It took a lot of practice, mostly via pattern recognition to lock-in the images up with concepts. The first time I was truly responsible for knowing an X-ray was on my Pediatrics rotation. There was a 2-week old neonate on our service, he was there for a fever and trouble breathing. As per protocol, reflecting current evidence and practice, the baby head a lumbar tap, labs, X-ray, the works. At some point, we narrowed it down to pneumonia involving the right lower lobe – that’s what I knew after calling the radiologist, and asking for a quick lesson in their interpretation. The mother stayed with her child day and night, the father would practically range from being at work to living at the hospital with his wife. Interestingly, the father was an attending at a prestigious hospital in New England. The mother of the patient wanted to have our team meet, when the husband was around, to explain our progress and plan. At our meeting with the family, I had to explain the X-ray to a doctor who most likely has been practicing longer than I’ve thought about medical school. I explained, he nodded a lot, and at the end everyone seemed relieved because we had a diagnosis. This is when I first though, “Radiology is kind of cool.”
Thus, for the last 4 weeks, I’ve been invested in all things radiology. We covered modalities to obtain images and impressions about the body and disease: X-ray, CT, MRI, nuclear scans, and ultrasound. We were allowed to go into any department we liked, such as Interventional Radiology, Mammography, and brain imaging rooms. We were even encouraged to eat, i.e. taste barium and gastrograffin (the former tolerable, the latter utterly disgusting). There were a couple of presentations, and we had to hold noon conference for the residents and attendings, for one day. Overall, it was a great experience.
My day started rather late, i.e. waking up at 7:15 AM for a 8:30 AM lecture. We usually would get out at 9:30 AM, then we had time to complete some mandatory accomplishments and assignments. We were required to go to three noon conferences a week, and two take one call evening. Our afternoon featured a second hour lecture, then we were free to do whatever we wanted with our time. Occasionally, I’d go back to a room to practice reading more scans with radiologists, other times I’d complete some of my treasure hunt of assignments, at other times (most of the time) I’d go home to study and relax. Patient interaction was very limited, typically only during procedures, or when someone looks lost in the hallways. Radiologist schedules are loaded to be efficient, a radiology interpretation can have a large impact on patient care and decisions. Thus, bottle necks of reads are to be avoided. So, the day and our schedules were just built efficiently. It requires a lot of background knowledge to read an image, that is something this rotation has taught me, after hanging out with radiologist for a month it’s obvious they spend a lot of their “free time” reading to become better radiologist.
Now, the best result of this rotation is that I can actually see stuff. I’m ready to use my newly received eyes for patient care.
Psychiatry Rotation – Over
It’s very difficult to summarize psychiatry. Prior to medical school, the world of psychiatry was rather murky to me. In fact, prior to starting the rotation I assumed that psychiatry issues were something you could parse-out, dissect, compartmentalize, and separate. They are not. Instead when speaking about the mind, psychiatry is like a baked-in ingredient – in a similar fashion, you’d be hard pressed to separate yolk from a finished cheesecake. About the body, well, I’ve spent over three years (plus) working on figure that little bit out.
The Case of Mr. Gibson
The phone rang, it was another order psychiatry consult put in. This time, to see Mr. Gibson, we were requested to check on a elderly war vet who had kicked a nurse that morning. On the psychiatry team, we lived in the locked unit. However, we were regularly consulted by different teams: medicine, hospice, and substance abuse units amongst others.
On the hospice care, Mr. Gibson had long ago heart disease and declining neural function had long ago robbed him of his independence. We made our way to his room and we solemnly approached his bed. In his prime, Mr. Gibson was a large man towering above others. But, in his bed, he appeared diminutive and a fragile in comparison to the gravitas he once held. I saw his personal affects surround his bed, an alter and praise from the people he loved. While maintaining the standard issue wards “listless face”, I internally grinned as I imagined him on his happier days. Helpless, we watched him fluctuate between deep hyperventilating breaths, shallow breathing, bouts of not breathing at all, his breathing accompanied by an intermittent rattle – proof that his central nervous system was struggling to regulate to handle his carbon dioxide – evidence that he was likely dying very soon.
The dialogue of the consult was always the same: build quick rapport, inquiry about mood, investigate consult concerns, determine the patients orientation, and figure out if the patient has been hallucinating, and most importantly determine suicidal or homicidal ideation. We gently woke Mr. Gibson for our consult.
The team: How are you Mr. Gibson?
Mr. Gibson: “I want to die…I have no regrets”, after another minute or two, I want to die…no regrets”
From his photos, he had lived a full life, he experienced love and marriage, the excitement and meaning of having children, probably the pain and growth of losing friends and family, at some point in his life the horrors of war, and the fortunate experience to come home after war. I thought of all of this, perhaps mainly to appease my own conscious, how else could I reconcile hoping that a patient soon passed away – some would say, “Go in peace.” Death itself is ambivalent, but the methodology can be cruel or benevolent. Seldom we get a choice of how we’ll go, but I was hoping his would be painless and on his time schedule.
Mr. Gibson died that very day.
Family Medicine Rotation Over
Two trains and an Uber, it was the same 2-hour commute to start my Friday at my family medicine assignment. My day started the same. Prior to meeting each patient, not having access to patient charts at home, I’d spend a little time reading up about them. At least, that’s how I hoped it’d go. Typically, I had very little, or absolutely no time to research a patient before having to present to an attending that love to start with, “So tell me everything you know about Mr. Wilson.” But, today, it was a rare exception. I knew this patient, in fact, I had sent her to the hospital a week earlier. I wondered what had happened to her.
One week prior, on a Friday, Ms. G, a 42 year-old RN visited our primary care office for what was labeled “same day sick visit.” Her history was significant for migraines. She hadn’t given any real details to the nursing assistant who booked the appointment. She had come in, with one of her daughters, she intended to make a quick visit and then bring her to lacrosse practice. The patient had her daughter wait for her in the lobby. As I took her vitals, I did the standard interview. And though rather reluctantly, the patient finally admitted that morning she experienced unilateral left-sided weakness in both her legs and arms, tongue heaviness, blurry vision, and “the worst headache” in her life. I took enough history to present a case to my supervisor that we should drop what we’re doing and get her ready to get picked up for hospital transport: raise clinical suspicions for stroke, mass, and an intracranial hemorrhage. Indeed, my supervisor did drop what they were doing to see the patient, we talked to the patient together. The patient, with reasonable denial, refused to go to the hospital. She had assumed it was just a severe migraine attack. She, a RN herself, was no stranger to the hospital system. The patient, my experienced than I, was no stranger to Occam’s razor – she knew the simple answer with the least amount of coincidences is usually the correct answer, thus given her history of recurrent migraines her theory of migraine attack held a lot of water. To the patient, I watched the nurse practitioner plead her best case of why she shouldn’t ignore her symptoms. I watched the patient skillfully, and thoroughly, brush off all of the medical advice. I was left alone with the patient, there was some awkward silence. I thought about not saying anything, her idea seemed logical, easier, and the patient gets what she wants: go along our day as if nothing happened. But, somehow I blurted out, “I know chances are you’re right, and I know this is a lot, but there’s a legitimate chance there’s something seriously wrong. And, I think you should go to the hospital. You need imaging, and you know that.” She didn’t say anything. Another awkward silence. She let out a sigh, and said “I know.”
So, I was somewhat excited to see this patient a week later. If I was right, awesome, I hope something treatable came of it. If I was wrong, she wouldn’t be admitted, she’d be hit with a nasty ED bill and potentially a bucket-load of imaging. I asked my supervisor if she had the paperwork from the ED on the patient, because while electronic health systems are usually updated into our systems hers was not. She gave me a little packet of paperwork and told me to read it before seeing the patient. Eventually, I got to the radiology report: 4x4x3 cm brain mass.
After reading the report, I called the patient to a patient room, we then sat down together. I asked how she was, and how much she knew about her admission and diagnosis. She was frustrated, angry, shocked, and overwhelmed. Who wouldn’t be? Being with her, in her dark moment, I remembered why I got into medicine in the first place. As I listened to her vent about the shock of the diagnosis, handed her tissues, and reviewed records with her, I remembered my goal is medicine is to help people continue on with their goals. To see people continue to be with the people they love, with the people who love them, and the people their love has yet to reach. This patient, a mother of three, wife, colleague in medicine, and most importantly a person, had a lot to live for. Indeed, the first visit with the patient involved physical medicine, while the second visit was a psychiatric mental health visit.
The visit ended, the patient and I most pick up the broken pieces, she went on with her life, and I went onto the next patient. That’s the strange thing about seeing patients, you see a tragedy, but you must see the next patient as if you’re unaffected and emotionally immune – the emotional Etch-a-Sketch. Everyone patient wants someone who cares, but not so much that it detracts from their care. And with that, my back to back visit transitioned from cancer to benign urinary tract infection. Only in family medicine could you go from talking about mortality to talking about the merits of cranberry juice.
My family medicine rotation is over, about 140 patients later, a wallet a lot lighter from transportation fees, another shelf exam on the books, and I’m two weeks into my Radiology rotation.
Best Wishes and Happy Thanksgiving
Pediatric Rotation — Over

About the format of this post, it’s sort of odd. Perhaps, one day, I’ll go back and editorialize this entry. For now, I’ll just stick with the facts my version of reality. Depending on the program, the Pediatric grade structure will vary. Most will have the same elements, clinical evaluations, activities you have to do, shelf exam or in-house exam. The shelf is a national, rotation dependent test, and an exam with standardized convoluted questions — because if they just asked you a straight forward question, and you answered correctly, where would the fun in that be? All of those elements, will be lumped and weighted together to form your grade: Honors, High Pass, Pass, and perhaps Low Pass. At my program, regardless of being on an away rotation, our grade is built mostly by evaluations from attending or resident physicians. In any event, this post will include some details about the structure of my Pediatric Rotation.
Location – a community hospital operated by Awesome General Hospital
Time – 6 weeks total, average work with 50 hrs (including didactics)
- 2 weeks on ED Pediatrics, mostly traige type of thinking; one on-call shift
- 1 week on Special Care Nursery, pre-round, round, write progress notes
- 3 weeks on Pediatric Inpatient Wards, gather vitals, round, check on patients throughout the day to assess the patient and how the plan is going, make lots of phone calls (talk to radiology to get help with a X-ray, make an appointment for the patient for follow-up care, talk to social workers; one on-call shift
- Weekly, half-day, ambulatory Pediatrics,
- One home visit to someone physically and/or cognitively disparity
Structure
The structure was dependent upon service and the whim of whoever attending I’m who’s on service.
ED Pediatric – this was my first excursion into Pediatrics, my patient loaded included whoever came in; however this service required very little management from my part as just about everything was algorithm based.
Types of cases: I saw the bread and butter stuff you expect to see: worried parents rushing in their newborns because of a fever (ending up with a urine analysis, blood work, and a lumbar puncture), concussions (I was usually given the task of telling the parents why we weren’t getting a CT), asthma, teenagers impaling themselves with objects (the oddest being a carabiner), sniffles, rashes, and one murmur that I got to diagnose and refer to cardiology for follow-up at Awesome General Hospital.
Structure: there were certainly lulls with nothing to do followed by bouncing around to room to room to see patients. Before seeing the patient, if I was lucky, I’d get the nurse’s “in-take note” (the reason why the the patient came, vitals, and a brief history when they were triaged). I’d walk into the room, introduce myself and role, get a quick targeted (but full) history of present illness and past medical history, do a review of systems, perform a targeted physical, then summarize an initial plan with the parents. The next step was to present the relevant parts of the case to my attending (there were no residents on this service, so medical students were the ‘residents’), and then I’d go over the plan that I thought of (aka winged) — the most important part of this conversation with the attending was to be efficient, they usually wanted a really quick explanation. Sometimes, we’d go back in the room together, the physician would do their own exam, repeating whatever they thought was worthwhile, and they’d either agree or modify my plan.
Summary: the cases were interesting, and I gained a skill at attending telepathy a.k.a. taking a guess at how much to summarize a case.
Special Care Nursery – my second service on this rotation. I was responsible for one to two patients per day.
Types of cases: as a newborn, you’re either put into a nursery if you’re healthy, a NICU if you’re really sick, or a special care nursery if you’re somewhere in between. As such, I saw and managed patients with prematurity complications, jaundice, failure to thrive, observation for murmurs and breathing difficulties, and neonatal abstinence syndrome (NAS). I took a special interest in the NAS babies, I had worked with mothers who were exposed to narcotics while pregnant during my Ob/Gyn rotation (some mothers were even from my home hospital in Boston, World’s Best Safety Net Hospital). So, it was a nice longitudinal experience. My previous rotation was Ob/Gyn, I learned a lot, but nothing about babies (or anything about children for that matter). However, I have a pretty good handle over pregnancy and woman’s health now, it helped that I’ve already been on the giving the baby away side of a birth. Now, on the receiving end of deliveries, performing neonatal resuscitations, the experience felt more complete.
Structure: again, there were no residents on this service, so you expected to perform a lot without much guidance. I’d pre-round on the babies, this essentially meant just copying down what happened over night in their paper chart (yes, I said paper). Then, I’d have about 15-20 minutes to get my thoughts together (aka scourer UptoDate and PubMed), and present the patient to the attending. At the end, I’d make an assessment and plan, sometimes they bought it sometimes they didn’t. After that, we’d round on the patient: check fontanelles, lungs, breathing, red reflex, check their oral cavity, and end with checking their hips for dysplasia. The remainder of my day was spent writing progress notes, most of that was rattling off a differential and justifying my final diagnosis. The day ended with the attending reading my progress note, making edits, and including my note into theirs — the most glorious moment was when an attending would just say, after signing off, “Just put your note into the chart”.
Summary: in a strange way, I enjoyed the neurotic level you have to go to manage special care unit babies. Not being satisfied with the patient monitoring my away rotations EMR had, I developed an excel sheet to finish better follow patients and write notes; I’m ashamed to say it brought out the “type A” in me.
Wards: my last service on Pediatrics, and the only part with residents; and arguably, it was the best way to end. I was responsible for 2 to 3 patients a day, depending on what was going on.
Types of cases: reactive airway disease, asthma, a bunch of pneumonia, croup, jaundice, liver problems, accidental (including some outrageous lead poisoning) or intentional poisonings, smoke inhalation after the patient’s family member tried to kill said patient, syncope, kids with seizures, and a spike in infants with viral meningitis. These were considered to be “bread and butter” cases to learn how to manage. If I had been at my home institution, or just back in my city, I’d probably see a lot of specialty cases and miss a lot of the “bread and butter”. That’s been the experience for some of my classmates who stayed in the medical capitol.
Structure: the name of the game is “family-centered-rounds“. The goal of family centered rounds, at least in theory, is to include the family into rounds. How family centered rounds play out, as I hear from residents, just depends on where you’re at and who s leading your team. In general, you present your patients in the room with the family, ask a few follow up questions, you explain the latest data to assess their child’s health, do a physical, and then tell the parents (or the patient only, if old enough) your assessment and plan for the situation. You leave the room, slip back into doctor lingo, and a period of critiques (positive and/or negative) and education starts (a.k.a. attending pimping). The rest of the day is spent making that plan you talked about come into fruition: leg work, working with the nurses, office stuff, and looking up a lot of things. Your patients on the floor who were admitted over night will need a full history of present illness note, so they can be properly admitted onto the floor. Your patients who you’re continuing to follow, or you’re covering, will usually only need a progress note. The only reason why I bring those notes up is that it’s a hell of a lot more work to finish putting together things for an admission than a progress note. Lastly, since the flow of the day was purely dependent on the whims of the attending physician, everything I said could be changed in any way they see fit — my biggest lesson, figure out what they want before you spin your wheels.
Summary: This rotation was sort of awesome because I learned how to better management patients and do doctor stuff. The difficult part about the this rotation however was differential diagnosis, i.e. the obscure stuff you didn’t learn about during the first two year of medical schools — heck, at best pediatric conditions and managements are foot-notes during the first two-years of medical school. Also, the intern and residents really improved my experience on the floor.
House visit: this was a one-time visit, we go in pairs (two medical students), and only a few medical schools in my city participate. You make one home visit to visit the family and patient as they deal with physical and/or intellectual disabilities — in my patient’s case, they had disparities in both. For my home visit, my patient was a teen with cerebral palsy (and bulbar palsy), and he required a computer to communicate with us. We spoke with the family about how this situation came to be, the affect their other children, how it affected their relationship as a married couple, and how they’re dealing with the finances. Last but not least, we got to know our patient.
Shelf Exam
Took the shelf today, next week I’ll know how I did. The exam is administered around the same time, in an official process, for many medical schools. Unfortunately, at least in our school and some others, our tests froze today on multiple occasions. This added about 30-40 minutes to our sitting time, while somehow syphoning off our test-time. In the end result, from our post test grumblings, was a reduction in time that left most of us with only a few minutes to 30 seconds on the last question. Fortunately, because I was skeptical about if the clock was running while my questions failed to load, I was too paranoid to take a bathroom break and ended up having a couple of minutes. For this exam, I used Pre-Test Pediatrics, Blue-Prints, some BRS, and a few slide decks gifted to me from others.
What’s Next?
Psychiatry at the VA! I’ve recently filled out a mountain of paperwork, I received an email today that I’m ready to go. I start this, after the weekend, this coming Monday.
That’s it for now, have a great weekend!
Ob/Gyn Rotation is Over
Hello,
So, in the midst of all the madness sweeping through the world, I’ve just finished the Obstetrics and Gynecology rotation — I finished my first rotation. I received some of my feedback from the interns, residents, and attendings; I was told that I made it to honors level if my shelf grade pans out (or a high pass at worse case).
Schedule and Experience
It was a 6-week rotation, 3-weeks on Gynecology and 3-weeks on Obstetrics. My hours of patient care, not counting charting, ranged from 12-17 hours a day, a typical day was around 14 hours with charting. After 6 weeks, I’ve seen and interacted with about 170 patients. Usually, once a week I had call. Interspersed within the rotations are ambulatory clinics. Once a week we had didactic days (lots of workshops about patient care and disease management), conferences, and one M&M meeting.
Ambulatory
- Student run clinic (we saw patients, diagnosed, and formulated treatment to be signed off by a physician or NP)
- Clinic for high risk pregnancies (gestational diabetes, mothers with risk of heart failure, etc)
- Substance abuse pregnancies (methadone, heroine, cocaine, etc)
- Gynecological Oncology
- Urology/Gynecology (usually pelvic floor dysfunction)
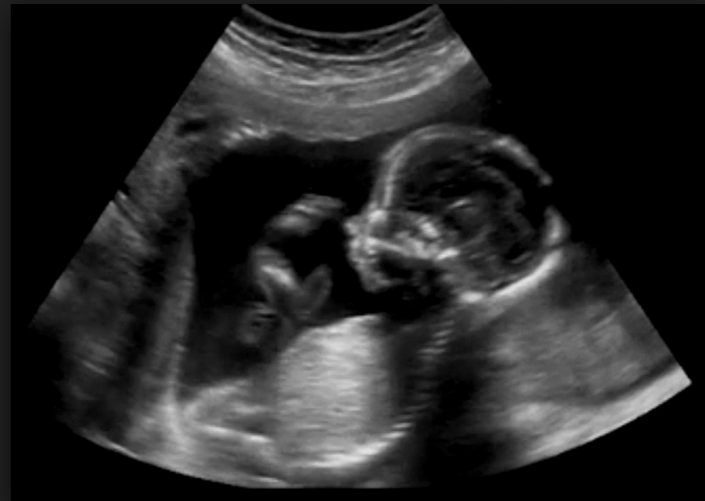
By the end of ambulatory Ob/Gyn, you’ll be a master of unsavory vaginal secretions, and you’ll feel unusually comfortable talking to women about their nether-regions. I’ve heard males have it rough, because some women don’t want their Gynecology care from them. Sure, there were a few patients who didn’t want me to do their vaginal exam. But, for the most part, after about two minutes of us talking and building up a relationship most women were very comfortable with me asking them questions and performing their exam. I only had one awkward experience that made me very happy I had a chaperone in the room. There was also an opportunity to an abortion. I was warned that seeing the fetus (at 10 weeks they’re rather human-like in form) could be traumatizing. After the abortion, you have to take the products of the abortion and identify the fetal parts: arms, legs, trunk, and head. Although, it may offend some people, this was actually less remarkable than I expected. The only thing that bothered me was the intense sucking sound during the procedure. On the other side of the spectrum, I’ll never forget using sonography to allow the mom to hear her baby’s heart beat for the first time — though, I’m not sure who was more giddy her or I, because it was my first time to do it.
Gynecology
Prior to this rotation, I was rather ignorant to the fact that gynecology is principally a surgical specialty. As such, you end up seeing a lot of procedures. In our program, you just signed up for whatever surgery you wanted to see. You’d follow that patient throughout their stay: do post-op checks, get to know their nurse, pre-round on them in the morning, present them during rounds, and make the occasional friendly visit just to see how they’re doing. When there’s downtime, you can study if you want, because it’s easier to remember a person than anything else I prefer to read up on the patient I have.
Pre-rounding: everyday, there are rounds, the most succinct description is people get together and talk about patients. Prior to rounds, because you’re expected to be an expert on your patient, you may (or must) pre-round on your patients. A lot of times, this involves getting in a little earlier to talk to the nurse that was with the patient overnight, waking the patient up to hear their subjective experience, doing a physical (including checking their wound healing, urine output, and overall disposition). Without a doubt, a lot of your conversation with the patient will revolve around you being excited that the patient had a bowel movement or passed gas. My biggest advice for pre-rounding is to get there very early, earlier the better, have your note down and practice it with your Sub-I or resident, then use your polished note as the basis of your presentation for rounds.
Surgeries: we could sign up for any surgery we wanted, as it was ‘required’ that a medical student is present for every surgery. Most people signed up for a variety of surgeries, hoping to never see the same procedure twice. Personally, after working with several surgeons, I signed up for the same surgeon repeatedly. This worked out for me, because there was a trust progression: first I was allowed to scrub in and successfully not touch anything, then I was allowed to assist in retraction, then I was allowed to suction and place a few stitches, and by the end allowed to diddle around with the laparoscope and help close with subcutaneous stitching. You learn a lot during the surgery, a lot of it applies to the shelf exam and to clinic (I’ll never forget that fibroid are a common cause of bleeding after my scrubs were soaked in blood during a surgery from the fibroid, even with the gown protection). My biggest advice for surgery, “Unless you know exactly what you’re doing, resist the urge to help”.
Obstetrics
This is exactly what you imagine it’ll be: pregnant moms, babies being flung into the cold hard world, and lots of fluids splattering on you. Child birth, at least the result, is rather beautiful. However, it shouldn’t be forgotten that for most women it’s the most dangerous and precarious event in their life. This is reinforced by the fact that in many countries, without modern facilities, labor and delvery is still one of the leading causes of death and morbidity.
Labor and Delivery: now I’ve seen a few vaginal births, I’d almost feel like a war criminal if I got a women pregnant — shout out to all the ladies who take one for the team and keep humanity going. But, I digress. This part of the rotation requires a lot of you, few things will inspire you to read-up than having to answer questions from anxious parents about their progress into labor. Labor and delivery was a mixture of organized chaos, calm (time to chart), and extreme organized chaos. Here, I’ve learned a few things:
- Holding a woman’s hand during contractions is helpful, but beware of women with long nails that dig into your skin.
- Babies either stubbornly are delivered cm by cm or rocket out like a cannon ball, it’s hard to predict which it will be.
- During delivery most fathers are rather useless, but them being there is usually better than not.
- Delivering the placenta is your job, as the medical student, it’s actually rather easy if you follow instructions but if you screw it up then the patient may exsanguinate — follow instructions
- A lot of people tacitly assume you know what you’re talking about, even if you don’t, so try to know what you’re talking about.
- Every women who chooses to give birth is gambling her life and such owns their experience, whether that be the decision to refuse an epidural or to refuse a c-section.
- Always have gloves in your pockets and also know where to find sterile gloves in a hurry.
Cesarean section: c-sections get a lot of bad press. Some think of it as ‘unnatural’, or a procedure overused by mothers too inconvenienced by vaginal births. But, I’d wager that if you’re fervently against c-sections you’ve 1) never given birth, 2) if you have, things ended without complications for you so you have biased perceptions, or 3) judging people is just your past time. It is true that the rates c-sections have risen, but so have the indications for c-sections: mothers at risk of maternal or fetal demise and/or morbidity. Though, it is disappointing when a mother who didn’t want a c-section ends up needing an emergent one to save their and/or their baby’s life. C-sections are a messy procedure, because birthing is a messy process: you’ll be squirted by amniotic fluid (fancy way to say baby pee), covered in blood, and bathing in your own sweat (the ORs are heated for the comfort of the soon to be delivered baby). Besides that, I’ll never forget reaching into a patients abdomen to manually contract an incompetent uterus with my bare hands, a uterus that wouldn’t have had the power to give birth vaginally. Nor will I ever forget seeing the umbilical cord tied in a knot and hence the indication for the c-section.
The most rewarding experience of any means of delivery is seeing the baby be put with the mom for immediate skin-to-skin contact. I still find it amazing to see the look on each mothers’ exhausted face, that look of relief and proud joy.
Grades will come out in a few weeks, hope I get honors. But, above all else, I’m really pleased with the experience and opportunity I was afforded. It was the first time nurses asked me for orders of what to do next, the first time I was thanked by a patient who referred to me as her doctor even though I told her I’m a medical student repeatedly, and it was the first time I’ve felt marginally competent in the entirety of medical school.
Next, onto Pediatrics (I see germs in my future).
STEP 1 No Longer Looms!
Hello,
I took STEP 1 yesterday! My perpetual 6 weeks of misery is over, also called ISP, the dedicated time we get to study for the exam. Some say “ISP” stands for Intensive Study Period, but over time I’ve heard it be called a lot of other things that also start with I.S.P. — I won’t repeat them here, it’s a PG website, but you can use your imagination. Over the years, STEP 1 has morphed, from a test you simply need to pass to one you have to do well on. There are a lot of grandfathered clauses like that in medicine, take the MOC for instance (the bane of the modern US physician). I don’t really think most of what I learned for boards is particularly useful, or even practical: can’t tell you how many lectures we had where seasoned physicians would say, I’ve never seen this in my life, but the boards seems to love to ask you about it.
About the exam, I felt like a decent amount I knew cold, some I had to work it out on the fly, and the rest I had to narrow it down and make an educated guess. Upcoming 2nd years have asked what I used, here it is:
- FA with DIT as a companion – DIT was a game changer for me, I’m thinking about using it for STEP 2.
- Sketchy Medical – the micro section is strong. Not the fault of the company, but some pharm sections are really hit or miss because people who name pharm drugs hate you.
- Pathoma – efficient, and really sticks to teaching.
- Lippincott Pathology – great for pictures you’ve never seen before, and getting used to recognizing gnarly things.
- UWorld – for the question bank for pathophysiology explanations and what not. For what it’s worth, the test format looks exactly like UWorld; though there were a lot less buzz words to bring you to a snap decision.
- BRS Physiology/Behavioral Sciences – I only did the problems, whatever I missed I’d go back and read in detail.
List amended 5/18 to include Lippincott and BRS
My biggest tip is listen to those in the class above you, they’ll know what your school failed to emphasize. Then find out what works for you, I really don’t think I should dispensing advice, after all I won’t even get my score back for 6 to 8 weeks. And honestly, even if I did well, STEP 1 prep is an individual experience and the questions you get are sort of random. My only advice, if any, is to study broadly and to keep your confidence up. They’ve changed the test format, there’s about 280 questions now, and with breaks, it takes 8 hours to complete. I used all of my break time, something I didn’t do during any of my practice exams (5 hrs). I was fortunate to have classmates to talk to during break, so it made each break session a good decompression. I brought a thermos of double shot of cappuccino that I made at home, lunch for fat and protein, and plenty of sugary snacks to give me a kick. I also brought enough Advil to ruin my organs, I popped one in the morning because I woke up with an intense headache after not sleeping too well during the night. I woke up several times, and drifted between stress awake and stress light sleep –apparently, my classmates who were also there that morning, also had the same experience. I was never a great sleeper, so it was to be expected.
Now, I have to sort out my life, get my financial aid in order, and complete some mandatory tasks before orientation starts. Next week, we do EPIC training (again for me), another TB test, pick up our pagers, and get our hospital patches to have sewn onto our white coats. My first rotation sent our on-call schedules, I’m scheduled 5 days on call for my first rotation. Besides that, we’ll get training how what to do if we’re jabbed with a needle, and meet our clerkship directors. Thursday, I’m going on vacation to New York (I haven’t left Boston since medical school started, except for a trip to Maine).
Lastly, it was cool to see the whole generation of test takers there, people taking their MCAT, STEP 1, 2, and 3 all in one center. Though, the person who was the most chill was definitely the guy taking STEP 3. It was a nice reminder of how far we’ve come.